|
|
Today in 2023 the number of new achievements cropping up each year is nothing short of astonishing. Modern medicine’s ability to heal previously unhealable parts of the body – from brains to hearts to compound fractures and nerve disorders – continues to amaze. Now, stem cell treatments are the newest addition to the healing repertoire.
Before diving into a stem cell treatment of any type, it’s important to note that almost all stem cell treatments remain in the experimental stages. For the small number of stem cell treatments that have been approved by regulatory bodies worldwide, even these treatments require meeting specific criteria before the patient is eligible for the treatment.
Almost without exception, the medical community is both excited and hopeful about the possibilities of stem cell treatment .
In this article:
- What Is Regenerative Medicine?
- What Is Stem Cell Therapy?
- 1. Non-Hodgkin’s Lymphoma
- 2. Leukemia
- 3. Stroke
- 4. Osteoarthritis
- 5. Rheumatoid Arthritis
- 6. Autoimmune Diseases
- 7. Spinal Cord Injury
- 8. Stem Cells for Hair Regrowth
- 9. Cardiac Problems
- 10. Diabetes
- Donor Cells: Autologous or Allogeneic?
- How to Approach Stem Cell Therapy Options
The 10 Most Popular Stem Cell Treatments
Stem cell technology promises to revolutionize the world of medicine and is now available in a number of forms, the top ten of which are listed below. Before we begin, it’s a good idea to take a closer look at what regenerative medicine and stem cell therapy involve.
What Is Regenerative Medicine?
Regenerative medicine is a field that would have seemed miraculous only two decades ago, much less two centuries. The basic premise is that, through various treatments, scientists and physicians can help patients who suffer from illness or injury to rebuild the affected parts of their body.
For instance, a patient who suffered a traumatic brain injury (TBI) could receive the necessary ingredients to rebuild the damaged parts of their brain. A person who was dying of cancer could receive new cells to replace the part of the body that doctors had to excise.
Regenerative medicine uses the body’s own ingredients – such as cells, structural tissue, exosomes, or other biomaterials – to repair damaged tissues and organs.
Stem cell therapy is one kind of regenerative medicine, and it holds a great deal of promise.
What Is Stem Cell Therapy?
The power of stem cells is that they are a renewable resource. As undifferentiated cells, they can turn into a wide variety of other cell types. Their power varies depending on how specialized they are, to begin with.
The main types of stem cells include:
- Multipotent stem cells: These cells are usually in one class, such as blood cells, cardiac cells, or nerve cells. They have the ability to turn into multiple types of stem cell within that class of tissues.
- Pluripotent stem cells: These stem cells have the ability to turn into any cell in the entire human body. However, until recently, these have only existed in embryos, the use of which has historically generated serious controversy. Luckily, new research has freed up pluripotent stem cells from much less polarizing sources, including donated cord blood from umbilical cords post-birth, and from adult stem cells. Science no longer needs to use embryonic stem cells, though they are still a valuable source of research and medicine.
- Totipotent stem cells: These are found only in the first few divisions of the human embryo. Such cells are a step above pluripotent because they can specialize not only in every cell of the human body but into placental and umbilical cells as well.
- Induced pluripotent stem cells (iPS cells): Researchers have developed new methods of turning adult cells into pluripotent cells by encouraging them to develop backwards from more specialized cells into less specialized cells. They do so through a variety of mechanisms and can harvest the starting cells from many places in the body.
Such a wealth of stem cell types, as well as the medical community’s growing ability to access them, has resulted in a powerful new technology for healing illnesses and injuries. Scientists and researchers have almost limitless ideas for the treatment of stem cells, which are currently in various phases of development.
Below are 10 of the most popular stem cell treatments right now. Most have not received FDA approval in the United States, nor approval from other regulatory bodies worldwide.
In this case, options are limited to:
- Participating in a clinical trial
- Seeking out stem cell clinics performing the procedure (without regulatory approval)
- Stem cell tourism (travel to a foreign country where the procedure is available)
The patient should use caution with all of these options. No matter which route a patient decides to go, it’s best to have a knowledgeable physician guiding your decision-making. That way, you can steer clear of any untested, suspect or dangerous treatments.
1. Non-Hodgkin’s Lymphoma
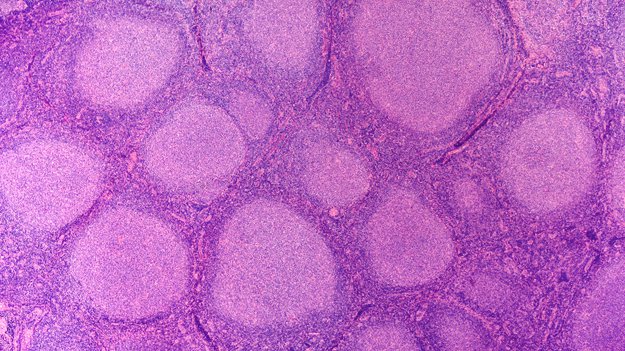
Non-Hodgkin’s lymphoma is a type of cancer that arises in the lymphatic system, which is responsible for fighting disease and toxins in the body. White blood cells, also known as lymphocytes, give rise to cancer cells, which then pervade the body. Without treatment, the condition is almost universally fatal.
Chemotherapy is an extremely effective tool against this disease. The problem is, high doses of chemotherapy often kill off bone marrow, in which new blood cells get made. In so doing, the chemotherapy kills cancer but also kills the patient, who now has no source of blood cells.
Stem cell treatment, however, helps mitigate this risk substantially by giving the patient an infusion of new cells following those necessarily high doses of chemotherapy. The patient first receives the chemo, then the stem cell infusion to help them repopulate their blood cell counts. Many patients show great promise of living long and healthy lives following the treatment.
2. Leukemia
Leukemia is another form of cancer that affects the lymphatic system as well as bone marrow. Leukemia cells are cancerous, affecting the immune system and causing an array of unpleasant symptoms, then eventually leading to death without treatment. It is the most common childhood cancer, but it affects adults of a range of ages as well.
Stem cell therapy poses significant hope, however. Much like with non-Hodgkin’s lymphoma, the treatment involves first killing off leukemia cells with high doses of chemotherapy and sometimes radiation as well. After the majority of cancer cells are defeated, the patient receives an infusion of stem cells to help the body repopulate, so that it can make normal blood cells once again.
This treatment, like the one for non-Hodgkin’s lymphoma, is typically only available to patients who have relapsed. That means their cancer went into remission from standard treatments, then returned months or years later. Good news, though: with a stem cell treatment within the first remission, the survival rate at 5 years is 30-50 percent. If the patient has not experienced a relapse within 2 years of the stem cell transplant, they have a good chance of surviving for many years.
3. Stroke
Recent research shows that stroke victims may find hope in stem cell transplants. An astounding study at Stanford University almost completely reversed the devastating effects of a stroke on Sonia Coontz, who suffered the attack on the brain at the young age of 31. After confinement to a wheelchair and speech difficulties for two years, she decided to enroll in a clinical trial, which used stem cells to rebuild centers in her brain.
Within hours of the stem cell treatment, she was able to move her arms and legs – whereas before she had suffered almost complete immobilization. She and her doctors also noticed rapid improvements in her speech – again, within only a few hours. Other patients noticed astonishing improvements as well, the only side effects coming in the form of “passing headaches.”
4. Osteoarthritis

Osteoarthritis is a degenerative condition affecting the joints. Over time, the cartilage that protects joints, preventing the rubbing of one bone on another, breaks down. Eventually, this can lead to the deterioration of the underlying bone as well, causing aching, stiffness, and eventual immobility in many cases. The condition commonly affects the hips, knees, and thumbs, though it can also strike elbows, wrists, ankles, and fingers.
The main issue with this condition is that cartilage is not a self-renewing substance. People are born with only so many cells in their bodies, which means that when those cells die and are carried off to the body’s waste disposal factories, no new cells take their place. Thus, the degeneration of joints and bones.
That’s where stem cells step in. Because they can transform into many different types of specialized cell, stem cells have the ability to become cartilage cells, renewing what was once unrenewable.
The procedure is offered in many clinics within and outside the United States and typically uses adipose cells as the stem cell source. Physicians extract these cells from fat tissue, separate out the stem cells from the rest, then prepare a solution containing growth factors and other ingredients necessary to tell stem cells how to develop in the new site. Once it’s prepared, doctors inject it into the affected site, such as a knee joint.
Regenexx is a U.S. company specializing in orthopedic applications of stem cells that was founded by Dr. Chris Centeno. Dr. Centeno is an expert in the clinical use of mesenchymal stem cells (MSCs) within orthopedic applications. His Regenexx clinic in Denver, Colorado, draws patients from all over the U.S. who are seeking innovative, non-surgical treatments for osteoarthritis, as well as a wide range of other orthopedic applications.
As the visionary behind the revolutionary Regenexx® technology, he pioneered a procedure that involves extracting a small bone marrow sample through a needle and a blood draw from a vein in your arm. These samples are then processed in a laboratory and the stem cells it contains are injected into the area needing repair. The goal is to deliver large numbers of stem cells to the injured area.
5. Rheumatoid Arthritis
Like osteoarthritis, rheumatoid arthritis affects joints. However, unlike osteoarthritis, which is a degenerative condition, rheumatoid arthritis is an autoimmune condition, in which the body attacks its own systems, causing destruction, limited function, and pain.
That means the mechanism for treatment is slightly different, with stem cell therapy potentially targeting the immune system rather than the joints themselves. That said, stem cell treatment of the joints can have the same positive effects as in osteoarthritis, and there’s no reason for patients not to try.
Clinical trials conducted in the last decade have not yet yielded conclusive results as to the efficacy of this treatment, but more trials crop up all the time, giving patients who struggle with severe pain and loss of mobility hope that they do may enroll in trials at home in the US or abroad. Example studies in Belgium have started, while some in the United States have wrapped up, with the scientific community awaiting information.
6. Autoimmune Diseases
Rheumatoid arthritis isn’t the only autoimmune disease, of course. A huge range of autoimmune conditions exists, such as diabetes, multiple sclerosis, lupus, Addison’s disease, Grave’s disease, and more.
These conditions all share the characteristic of the body’s immune system reacting to normal substances in the body as though they were pathogenic. That means instead of letting the body function normally, the immune system will attack tissues and substances, creating ongoing sickness and in many cases, eventually death.
Stem cell therapy has two possible benefits in the case of autoimmune diseases. For one thing, it can help repair and regenerative tissues damaged in an autoimmune attack. Stem cells can help them repair nerves, skin, blood, organs, and more. This helps the patient regain their health and fight the degenerative nature of such diseases.
Second, stem cells can actually modulate the immune system so that it no longer attacks the body so viciously – or at all. Research demonstrates that stem cells can minimize the pathological effects of the immune system, making it so the body no longer attacks itself – all while preserving its ability to attack foreign substances and real pathogens.
7. Spinal Cord Injury

One of the most traumatic injuries to the human body is blunt for trauma to or severing of the spinal cord. Depending on where the injury occurs, the patient may never walk or even move their arms again. For most of human history, such a traumatic injury was completely irreparable. In recent years, neurosurgery has given people back some of their function in cases like these, but outcomes are still all too often disappointing.
Stem cells provide serious hope for the future. Instead of trying to repair damaged nerves, stem cells offer the ability to replace them. By injecting stem cells to the site of the injury, the spinal column can repair itself, accessing all the ingredients it needs for the specialized job.
In combination with growth factors and hormones, stem cells are capable of traveling to the site of the injury “assessing” what needs rebuilding and stepping in to do the job for doctors. This limits the number of modifications needed from the outside and leaves the healing to the body.
While the mechanisms aren’t yet clear, it seems that hormones such as growth factors – in addition to the location in the body – can provide signposts to stem cells telling them what kinds of tissues are needed. Then the stem cells transform into them, integrate with the damaged tissue and repair it.
8. Stem Cells for Hair Regrowth
While balding is far from life and death, many people care about their hair a great deal. Luckily, stem cells are paving the way for all-natural hair regrowth.
The simple outpatient treatment may actually provide the de-balding effects for which men and women have searched for decades (scratch that: centuries). Here’s how it often works: The patient goes into a clinic. The specialist removes follicles from their scalp, separates out the stem cells, and injects those follicles along with stem cells back into the scalp.
Recent research in Italy has developed one mechanism of doing so, while multiple clinics across the United States, Europe, and other locations worldwide offer modified versions of the treatment. The essence of the therapy involves encouraging formerly hairless or balding sections of the scalp to grow by offering the nutrients needed to regenerate hair and a follicle needed to produce one in the first place.
A leading company working on a treatment for hair loss is Replicel. Headquartered in Vancouver, Canada, the company is developing an autologous cell therapy utilizing dermal sheath cup (DSC) cells to treat androgenetic alopecia (male pattern baldness). The product that Replicel is developing is called RCH-01. It is poised to begin a Phase 2 trial that will enroll 160 male subjects.
In the trial, dermal sheath cup (DSC) cells will be isolated from a biopsy taken from the back of the patient’s head. Afterward, the cells will be multiplied in the lab and injected into balding areas on the patient’s scalp.
Before embarking on a hair treatment plan, be sure to research the clinic. Although stem cell treatments for hair loss are certainly available, they are not approved by the FDA and are at this point considered uniformly investigational. That means patients shouldn’t conclude they’re safe based on a few website testimonials. Do the research and, as always, speak with a physician before signing on the dotted line.
9. Cardiac Problems
Heart disease is still the No. 1 killer in the United States (although by some estimates cancer will soon or has already surpassed it). For obvious reasons, stem cells seem like a strong possibility for repairing heart tissue and helping to overcome the intermediate symptoms that eventually lead to heart disease or cardiac arrest.
As is the case with most of these therapies, the biggest benefit of stem cell treatment for heart disease is its ability to replace damaged or dead cells without the need for invasive surgery or transplants. An injection of stem cells can give the body the ingredients it needs to grow the specialized cells on site, ideally without having to put the patient under or open them up. The exact mechanisms of this procedure are not as yet clear, however.
On 16 May, 2018, Nature News reported that Japan’s health ministry gave doctors at Osaka University permission to take sheets of tissue derived from stem cells and use them to treat diseased human hearts. From preclinical studies in pigs, it appears that thin sheets of cell grafts grown from induced pluripotent stem cells can improve heart function. While the treatment approved by Japan’s health ministry will only be tested in three patients, a follow-up trial could enroll ten or more patients.
Stem cell therapy for heart disease is currently limited to clinical trials.
10. Diabetes
Many people are very interested in the possibility of stem cells to treat diabetes. Both Type I and Type II diabetes have devastating effects on the health of millions, and stem cells may help to ameliorate those conditions.
Type I and Type II diabetes affect the body in different ways. Type I diabetes is genetic, and results from the pancreas failing to produce insulin, or producing too little of it. Insulin is what tells the body to remove glucose from the bloodstream and let it into cells, so they can use it for energy. Most likely this is due to an immune system disorder in which the body attacks its own islets, the pancreatic cells responsible for manufacturing insulin. In this case, stem cells may provide the same immune system-modulating effect as they do for other autoimmune diseases.
Type II diabetes is when the body becomes resistant to insulin. The pancreas may still make it, but the patient’s body does not sense it – it is “insulin resistant,” which means the release of insulin in the bloodstream still does not result in cells taking up glucose. It remains in the bloodstream, causing dangerous hyperglycemia just as it does in the case of Type I.
The second condition may also respond to stem cell treatment, which can help moderate pancreatic productive of insulin as well as helping the body respond to it more effectively. Multiple clinical trials assessing the validity of stem cells for both diseases are underway, and many eagerly await their results.
Given the growing promise of regenerative medicine, it is not surprising that fourteen companies are now exploring cell therapy approaches to the treatment for diabetes.
Donor Cells: Autologous or Allogeneic?
There exist two possible sources of stem cells: autologous and allogeneic. Both provide benefits and drawbacks.
Autologous stem cells are those that come from the patient’s own body. Physicians can source them anywhere, from blood or other tissues, but they still count as autologous so long as the patient themselves is the source and recipient of the stem cells. Allogeneic stem cells, on the other hand, come from donors – usually family members, but sometimes anonymous donors who have given their stem cells to a bank.
Autologous stem cells are ideal since the body already “knows” the cells and doesn’t consider them invaders, as is often the case with donor cells. There is a very little risk, therefore, of the patient rejecting the stem cell infusion (except in rare cases where the patient has an allergic reaction to a preservative or other agent used in preparation). There is also no risk of graft-versus-host disease, a condition in which the donor cells from another individual see the patient’s body as an “invader” to the donor’s immune system, and will, therefore, attack it.
So why doesn’t every stem cell patient use autologous cells, then? Usually, it’s due to the danger that the patient’s own cells will re-infect them with a disease. For instance, in the case of leukemia or lymphoma, the patient needs cells other than their own to ensure no reintroduction of cancer cells. That’s why donor cells are critical – but again, they do bring risks.
Overall, the decision is a very personal one that patients should discuss with their managing physicians before taking action. Note that in cases where allogeneic cells are needed, it can take a long time to find the right donor, so it’s best to start as soon as possible.
How to Approach Stem Cell Therapy Options
Not all treatments are equally available to patients, nor will they necessarily provide the same results across the board. Whether or not a certain therapy is right for a patient depends on many factors, including:
- Their age and the general state of health
- The illness or injury which the stem cells must address
- Where they live
- What kind of support they have during and after treatment
- What other types of procedures must occur at the same time
- Whether the patient can use their own cells or must use others’
- What studies say about the treatment
- Who is available to treat the patient
- Their willingness to undergo the difficulties and side effects of treatment
…among other factors.
The best approach in cases where the studies have unclear results and the patient isn’t sure where to turn is to speak with a physician. They will have much better guidance to offer than one can find online, and can help prepare the documentation needed to enroll.
Patients and loved ones can also speak with clinics, who often provide stem cell treatments of the types discussed above, with patients reporting significant positive results. Beware, though, that terms like “human trials” and “human studies” get tossed around rather loosely these days. Technically, a clinical trial must follow an array of very specific guidelines to constitute a valid form of medical research. It is a time-consuming process to start and fund a clinical trial, so before enrolling, always do due diligence.
Stem Cell Treatments
If you are seeking a stem cell treatment, we recommend GIOSTAR to help you access medical guidance and advice. In alignment with what we believe at BioInformant, GIOSTAR’s goal is to offer extensively researched stem cell therapy options designed to improve a patient’s quality of life.
Click here to Schedule a Consultation or ask GIOSTAR a question.
If you found this article valuable, subscribe to BioInformant’s stem cell industry updates.





















Anyone try stem cell therapy on hereditary spinocerebellar Ataxia yet?
I don’t seem to be able to find much info on neck stenosis or any kind of success with cervical stem therapy.
Are there any clinical trials for Hypoxic/ Anoxic brain injury?