|
|
What is platelet-rich plasma (PRP)? It is a product that is derived from a patient’s own blood which contains a concentration of platelets and growth factors, which are pro-regenerative factors. Today, platelet-rich plasma (PRP) therapy is been used across a range of medical fields, including orthopedics, dermatology, and sports medicine, to promote healing and tissue regeneration.
How Does PRP Work?
PRP, short for platelet-rich plasma, is a convenient treatment option for many soft tissue injuries, because it only involves a blood draw from the arm. The blood is spun down in a centrifuge, separating out the platlet rich plasma (PRP) portion in which there are concentrated growth factors and cytokines.
This process separates the platelet-rich plasma (PRP) component of the blood from the red blood cells and other non-therapeutic components, producing a concentrated source of self-derived (“autologous”) platelets as the final PRP product.
This resulting PRP component contains both growth factors and cytokines that may have ability to support or stimulate healing of bone, as well as soft tissue structures, such as ligaments, tendons, fascia, and more. While there have not yet been large-scale, controlled clinical trials conducted to evaluate the efficacy of PRP, the procedure has nonetheless become commonplace in medical offices worldwide, most frequently within orthopedic offices.
The growth factors and cytokines then work as signaling factors within the area they are injected.
There is scientific evidence to suggest that these components may facilitate repairs of soft tissues, but the exact method of action is not fully clear.
Can PRP Therapy Activate Stem Cells?
There is also good evidence to suggest that PRP activates stem cell activity, which is why it is sometimes recommended before and after getting a stem cell treatment. For example, BioInformant’s Founder received a stem cell treatment for an orthopedic injury and it involved getting a PRP application prior to the stem cell treatment to boost the regenerative potential of the treatment.
Specifically, studies have indicated that PRP therapy may have the ability to increase stem cell quantities, as well as to assist stem cells with facilitating natural healing processes.
In a recent October 2016 study by Sakata R, Reddi, et al., the researcher team conclueded that PRP therapy may modulate regeneration of articular cartilage and retard the progression of osteoarthritis (OA) by stimulating cell migration, proliferation, and differentiation of stem and progenitor cells.
Similarly, a September 2016 study by Teng, et al., found that when PRP therapy was administered in combination with bone marrow stem cells, it promoted difficult to treat tendon-bone healing in a rabbit model of anterior cruciate ligament (ACL) reconstruction.
Clearly, there are some interesting indicators that PRP and stem cells may be synergistic in their activity.
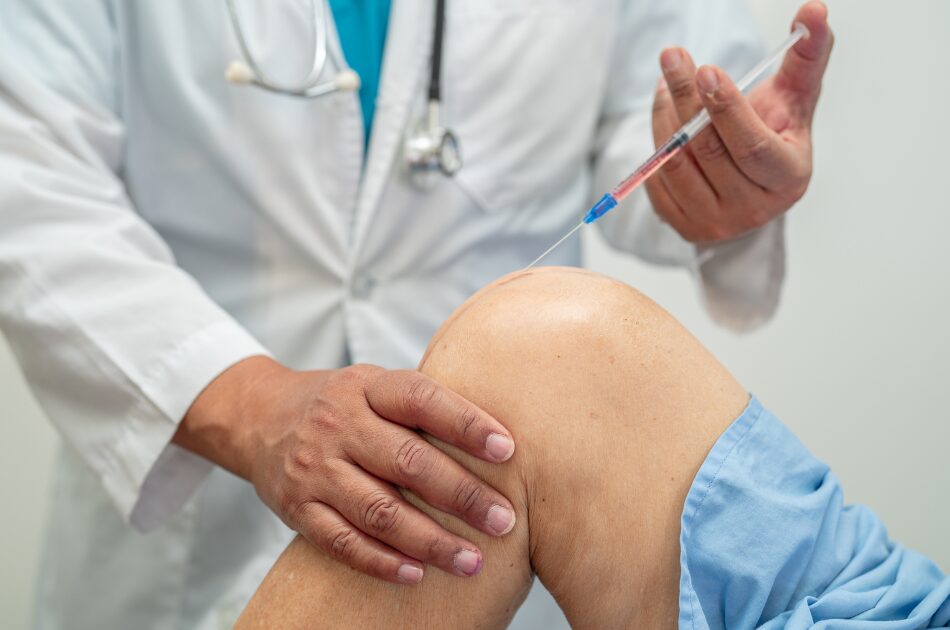
When is PRP Most Often Utilized?
PRP is now widely utilized for a wide range of human applications, including the following:
- Sports Medicine
- Orthopedic
- Spine
- Oral & Maxillofacial(OMF)
- Cosmetic/Aesthetic
- Pain Management
- Traumatic Injury
- Chronic Disease
When Does PRP Work Best?
It is important to understand that PRP “induces” repair through growth factors and cytokines and does not actually reconstruct damaged tissue. Therefore, it works best on minor-to-moderate injuries.
Specifically, PRP therapy has shown promise for the following situations:
- Musculoskeletal Injuries: To date, PRP has been widely used to in the treatment of tendon injuries, such as tennis elbow, Achilles tendinopathy, and rotator cuff injuries. It can also be used for osteoarthritis in joints such as the knee, hip, and shoulder.
- Soft Tissue Injuries: PRP injections may help accelerate the healing process in soft tissue injuries like ligament sprains, muscle strains, and other types of tissue damage.
- Dermatological Conditions: PRP therapy is used in dermatology for various purposes, including hair restoration, skin rejuvenation, and wound healing. It has shown efficacy in promoting hair growth and improving skin texture and tone.
- Surgical Procedures: PRP can be used to enhance the healing process after certain surgical procedures, such as joint reconstructions or tendon repairs.
- Chronic Conditions: PRP therapy may benefit patients with chronic conditions, such as osteoarthritis, where traditional treatments have been less effective.
It’s important to note that the effectiveness of PRP therapy can vary substantially depending on factors such as the specific injury or condition being treated, the patient’s overall health, and the technique used to prepare and administer the PRP. Additionally, more research is needed to determine the long-term effectiveness of PRP therapy. For this reason, patients considering PRP therapy should discuss its potential benefits and risks with their healthcare provider and ensure that they have realistic expectations about the outcomes. As with any medical treatment, not all patients will experience significant improvement with PRP therapy.
Given this context, PRP could be an intelligent and minimally-invasive treatment approach to try if you can get healthcare coverage or are willing to pay the costs out of pocket. This is because the primary downside is the cost, which typically ranges from $300 to $1,500 or more per treatment.
If you found this blog valuable, subscribe to BioInformant’s stem cell industry updates.

Tell Us What You Think!