|
|
Embryonic stem cells are cells that can give rise to all of the tissues types that form a human being. These stem cells are being used in drug development, toxicology testing, and disease reversal, as well as to grow healthy new tissue to heal injuries.
While they are powerful cells, embryonic stem cells are controversial to produce, because they are created from human embryos. For this reason, they have limited use and receive restricted funding. Learn more about these cells below.
Embryonic Stem Cells and Their Uses
In this article:
- What are Embryonic Stem Cells?
- Embryonic Stem Cell Pros and Cons
- Human Embryonic Stem Cells
- What Is the Timeline of Harvesting Embryonic Stem Cells?
- History of Human Embryonic Stem Cells Research
- The Significance of Pluripotent Properties
- Totipotent, Pluripotent, and Multipotent
- Potential for Treating Disease
- Potential for Medicinal Research
- What Types of Stem Cells Exist?
- What About Adult Stem Cells?
- The Future Of Stem Cell Therapy
What are Embryonic Stem Cells?
Embryonic stem cells are unique cells that exist in an early-stage embryo. During pregnancy, they develop into all of the cells and tissues that form the fetus and the newborn it grows into.
Embryonic or otherwise, stem cells differ from other types of cells and represent a fraction of the trillion of cells that compose the human body. Unlike regular cells, embryonic stem cells can reproduce. They can also turn into different kinds of cells, known as differentiation.
These pluripotent stem cells boast special characteristics that often make them better suited for therapeutic purposes than adult stem cells. It’s helpful to remember that “adult” stem cells can also refer to those in newborns and children. The term simply means that the cells are sourced from a human being after a live birth This makes adult stem cell types non-controversial.
Embryonic Stem Cells Pros and Cons
The embryos used to create embryonic stem cells come from in vitro fertilization clinics. These embryos would have otherwise been destroyed or discarded as medical waste by the fertility clinic, because they were not chosen for implantation into a mother or surrogate.
Because they are created from embryos, some people are opposed to research involving embryonic stem cells. Other groups, like the Michael J. Fox Foundation, have been highly favorable toward embryonic stem cell research, because the cells are versatile and have great potential for use in regenerative medicine to cure a range of diseases that burden the human race, such as Parkinson’s disease, Alzheimer’s disease, multiple sclerosis (MS), and more.
To gauge what percentage of the public supports embryonic stem cell research, BioInformant posted a Twitter poll. The results of this poll are shown below, showing that slightly more than half of respondents support embryonic stem cell research (58%) and an astounding 84% of respondents either support embryonic stem cell research or think it depends on the situation.
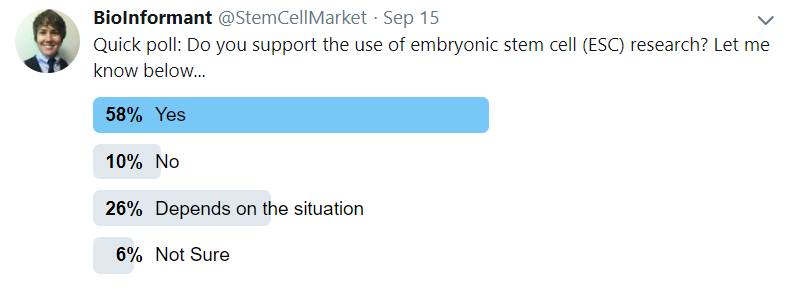
Human Embryonic Stem Cells
Human embryonic stem cells (hESCs) are pluripotent cells that are derived from embryos at fertility clinics and provided with informed donor consent. Embryonic stem cells are usually harvested shortly after fertilization (within 4-5 days) by transferring the inner cell mass of the blastocyst into a cell culture medium, so that the cells can be multiplied in a laboratory.
Pluripotent cells can give rise to all of the cell types that form the human body, making them very powerful for use within regenerative medicine applications.
As the name suggests, human embryonic stem cells are derived from human embryos, which makes them controversial to produce. Thankfully, these cells are only produced from embryos that would otherwise treated as biological waste produced as a byproduct of the assisted fertility process at fertility clinics.
In contrast, embryonic stem cells can also be derived animal sources, such as from mice, rats, monkeys, and more. These animal derived embryonic stem cells are substantially less controversial for use in research applications. Unfortunately, they also have few therapeutic applications, because there are immunological issues associated with using animal cells within humans.
What Is the Timeline for Harvesting Embryonic Stem Cells?
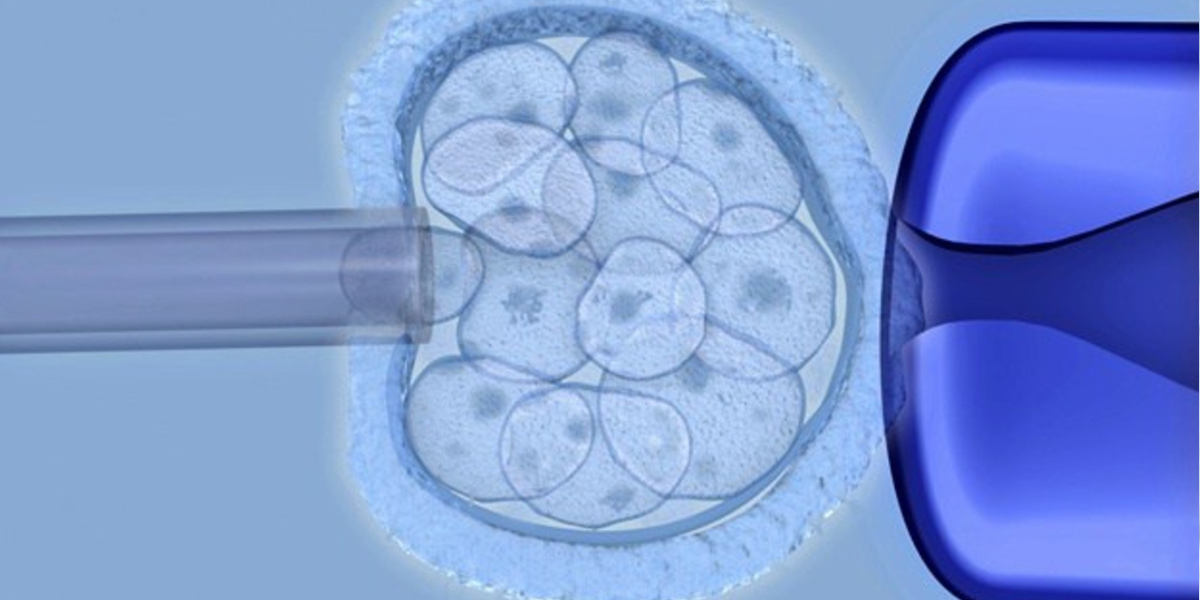
Researchers harvest human embryonic stem cells from a blastocyst. That’s the scientific name for an embryo in its earliest form, usually 4-5 days past the fertilization stage. In traditional human pregnancy, the blastocyst stage occurs before the embryo reaches — and implants within — the mother’s uterine wall. At this blastocyst stage, the young embryo has about 150 cells. That makes it easy to isolate them for harvesting.
Blastocyst embryos used for harvesting come from embryos created in fertility clinics, not from a woman’s uterus. Researchers harvest them with the permission of the sperm and egg donors. Once created, the blastocyst embryos can be preserved indefinitely under laboratory conditions.
Researchers harvest the embryo stem cell at the Day 4 or 5 stage. This time frame is crucial, because it is just after the embryo begins dividing multiple cells within itself, but before those cells begin to differentiate.
To differentiate, as the name suggests, means that the cells begin to become specific to one of the three germ layers. However, an inner cell mass (ICM) does form, within a protective outer layer. The cells get harvested from the ICM after scientists penetrate the outer layer.
History of Human Embryonic Stem Cells Research
Scientists first isolated embryonic stem cells in mice in 1981. Much later, they isolated human embryonic stem cells in 1998. Ethical concerns caused much of that gap in research. For moral and practical reasons, the cells needed to be harvested from embryos that didn’t come from a pregnant woman.
Fortunately, by the late 1990s fertility clinics perfected many new techniques. Those breakthroughs not only meant higher success rates for hopeful couples, they also created more viable embryos from which stem cells could be extracted. The clinics reportedly had about 11,200 embryos in frozen storage that would otherwise be discarded. Instead, the clinics donated some for stem cell research.
Scientists cleared the second major research hurdle in 2001 when the federal government decided to fund embryonic stem cell research. This support allowed various research facilities to obtain and study the embryos.
The breakthrough came at an exciting time, because researchers had only recently learned how to extract the needed embryonic stem cells. The mouse-related discovery in 1981 was important. However, those cells differ too much from human embryonic stem cells to put the knowledge to use. In the interim, researcher achieved breakthroughs with other primates.
The Significance of Pluripotent Properties
Scientists value embryonic stem cells because of their pluripotent properties. For the non-scientists among us, that means they cells are highly versatile and capable of becoming a wide range of cell types. Many stem cells can only produce exact copies of themselves — for example, blood cells to blood cells, bone cells to bone cells, and so forth. a pluripotent stem cell is defined as a cell that can change itself into nearly any cell or tissue type within the human body.
In practice, this allows scientists to turn embryonic stem cells into any part of the body. Cells develop in layers, known as germ layers. Humans have three germ layers. The outermost, the ectoderm, consists of skin and nervous system. Next, the mesoderm, make up bones, blood, muscles, and the genial system. The innermost germ cell layer, the endoterm, includes lung and digestive system cells. Taken together, adult humans have 220 different types of cells within those three layers.
Embryonic stem cells keep generating new cells, making them useful. These reproductive abilities mean the stem cells ultimately form tissue to can be used to help patients. The tissues can also be used by scientists to conduct medical research.
Totipotent, Pluripotent, and Multipotent?
While embryonic stem cells are pluripotent stem cells, there are also two other types of stem cells: totipotent and multipotent cells. What is the difference between they cell types? The answer is simple.
Totipotent stem cells are the most versatile stem cell type, because they are formed shortly after fertilization of an egg cell by a sperm cell. They can become all of the cells of the human body, as well as the cells of the embryo and developing fetus. At about four days into development, these totipotent cells specialize slightly, becoming pluripotent stem cells, such as the embryonic stem cell.
Later, multipotent stem cells form, which are again more limited in what they can become. They cells types usually prefer to become cells of a certain class or category.
For example, hematopoietic stem cells (HSCs) are a type of multipotent stem cell that prefer to become cells of the blood and immune system, although it it possible to induce them to become other cell types.
Potential for Treating Disease
Scientists only recently began to understand how many diseases and conditions embryonic stem cells may be able to treat. Research is still ongoing. Because so many health problems involve the dysfuntion or death of cells, human embryonic stem cells may be able to reverse the progress of these diseases.
In the future embryonic stem cells may contribute to the treatment of Parkinson’s disease, heart disease, diabetes, spinal cord injuries, vision problems, or other diseases and conditions.
Potential for Medicinal Research
Suitable subjects for testing present a major stumbling block toward radical breakthroughs in pharmacology. Early versions of medicinal drugs and surgical procedures carry potential side effects that may not come out until testing actually occurs. This is obviously problematic for any human subjects, especially for those already frail from the disease or injury.
That is why human embryonic stem cells present a radical opportunity for new breakthroughs in drug therapy and surgical procedures. Scientists can grow healthy tissue from embryonic stem cells to see how that tissue responds to these therapies. They can also give that tissue specific disorders, then attempt to “cure” it with new medical breakthroughs.
Human embryonic stem cells have the ability to transform into other cells. From those new cells, scientists can create heart tissue, bone marrow tissue, blood samples or other body parts which they need to test. In doing so, they can avoid experimenting on patients.
What Types of Stem Cells Exist?
In addition to embryonic stem cells, several broad categories of stem cells exist.
A complete list of these stem cells types is included below:
- Embryonic Stem Cells (ESCs) – This is the only controversial stem cell type. ESCs are derived from blastocysts, a stage within the developing embryo. As described earlier, they can differentiate into any cell or tissue type within the body.
- Perinatal Stem Cells – Perinatal stem cells are cells which are obtained during the period immediately before and after birth. Collection of these cells does not impact the fetus or newborn, so they are non-controversial.
- Adult Stem Cells – These are non-controversial cells present in the tissues of live adults. Everyone has stem cells present in their bone marrow, fat (adipose tissue), dental pulp, peripheral blood and more.
- Induced Pluripotent Stem Cells (iPS Cells) – iPS cells were discovered in 2006 in mice and in 2007 in human. They cells are non-controversial, because they are adult cells that are created in a lab through genetically reprogramming. Like embryonic stem cells, they can become any cell within the body.
- Cancer Stem Cells (CSCs) – Cancer stem cells are a type of stem cell that appear to play a role in tumor formation and potentially cancer progression.
Stem cell research has been going on for over 50 years because stem cells have a unique ability to divide and replicate repeatedly. In addition, their unspecialized nature makes them of great interest for regenerative medicine applications.
What About Adult Stem Cells?
Adult stem cells also hold more great promise. In healthy humans, adult stem cells produce new cells when needed, to maintain normal functions and repair minor wounds and disorders. However, they are considered less versatile, because they cannot differentiate into all tissue types that compose the human body like embryonic stem cells.
Adult stem cells typically have a preference to become certain tissues within the human body. For example, hematopoietic stem cells (HSCs) are a widely researched adult stem cell type. Although HSCs prefer to become cells of the blood and immune system, they can sometimes be coaxed to become other cell types.
Another example of the utility of adult stem cells is the success of bone marrow transplants. Bone marrow transplants treat patients with cancer whose immune systems have been compromised by chemotherapy or radiation. A bone marrow transplant from a donor — or from the patient, prior to treatment — uses bone marrow stem cells to help generate new cell production.
The Future of Stem Cell Therapy
Over time, researchers have discovered adult stem cells in many sites throughout the human body. Adult stem cells are now known to exist in the blood, bone marrow, fat (adipose) tissue, dental pulp, neural tissue, and many other sites.
These stem cells are capable of positively affecting a wide range of diseases through either tissue repair or signalling mechanisms. Particular stem cells types, like mesenchymal stem cells, can lower inflammation, reduce scarring, and improve immune function.
What changed? Until recently, adult stem cells were considered inherently limited, because they do not differentiate into all of the cells that compose the human body. However, researchers have found a variety of ways to activate both cell division and differentiation. This ability to grow more healthy tissue in laboratory conditions could substantially alter the future of medicine.
Access to embryonic stem cells is inherently limited to the number of available samples from fertility clinics. Yet adult donors are more plentiful. This is particularly true if a patient can act as his or her own donor.
Seeking Stem Cell Treatment?
As the world’s largest publisher of stem cell industry news, we understandably cannot provide clinical treatments or advice. If you have medical questions, please contact GIOSTAR, a global stem cell company that has treated a large number of patients.
You can reach GIOSTAR at this link to schedule a consultation or ask them your questions.



















Yes I support using it.