|
|
Lung diseases can be debilitating, making both medical leaders and patients interested in exploring stem cell treatments for lungs. Find out what you need to know about stem cell therapy for lungs, including risks, benefits, clinical trial progress and more.
Stem Cell Treatments For Lungs
In this article:
- Progression of Treatments for Lung Diseases
- Where Do Stem Cells for Lungs Come From?
- How Do Scientists and Physicians Harvest and Use These Cells?
- Risks of Stem Cell Treatments for Lungs
- Benefits of Stem Cell Treatments for Lungs
- Lung Stem Cell Clinical Trials
Progression of Treatments for Lung Diseases
Historically, those with Chronic Obstructive Pulmonary Disease, also known as COPD or lung disease, had only a matter of time before they succumbed to symptoms. These include wheezing, chest tightness, mucus in the lungs and death. The same is true for lung cancer, which kills hundreds of thousands each year (an estimated 135,720 deaths in 2020, according to the American Cancer Society).
Recently though, a beacon has broken through the fog. Stem cell treatments for lungs are showing promise for treating lung diseases, most notably COPD and non-small cell lung cancer (which does not metastasize nearly as quickly as small cell lung cancer). Mounting research shows that stem cells can also make a difference in pulmonary fibrosis.
However, the new treatments raise many questions. Where do these stem cells come from? How do physicians use them to repair lung tissue? What are the risks and benefits? Lastly, what can one do to join clinical trials?
The following will attempt to answer these questions, so that those with lung diseases or their loved ones have the necessary information to make choices regarding future treatments.
Where Do Stem Cells for Lungs Come From?
While some people associate stem cells with unborn fetuses, the adult human body actually provides many rich sources of stem cells. They exist in the blood, muscles, skin, liver, brain, bone marrow and even teeth.
Some of these stem cells are very flexible. Hematopoietic stem cells, for instance, can turn into a variety of cell types that compose the human blood and immune system. Mesenchymal stem cells are a type of multipotent stromal cell that can also turn into many different types. They can transform into muscle cells, bone cells, fat cells, and cartilage cells, among others.
However, adult stem cells that can transform into lungs have posed notable trouble to researchers and physicians. Not only do lung cells turn over slowly – making the lungs hard to heal – but they are difficult to find. Now, studies have demonstrated that lungs actually do contain several populations of lung stem cells.
According to the National Institutes of Health, researchers have identified a new type of stem cell. This stem cell produces new critical ways to support the function of alveoli or air sacs, which inflate and deflate, allowing the lung to exchange gas.
Another example of lung stem cells is the c-kit-positive lung stem cell. Progenitor cells, which are like stem cells in that they can give rise to multiple types of cells but are much more “niched” in what they can become, are also abundant and can contribute to treatment.
The most promising lung stem cells are called alveolar epithelial progenitor (AEP) cells. They are relatively easy to isolate from adult lungs via the use of a surface marker, which attaches to only that type of cell. Once detected and harvested, physicians can use them to develop new populations of cells.
How Do Scientists and Physicians Harvest and Use These Cells?
Once physicians have stem cells in hand, they can inject them into the patient. Once inside, they will theoretically – if all goes well – repopulate inside the patient’s body, replacing the damaged cells. In vivo studies of mice have so far proved promising, showing that injected stem cells do indeed “take” and work to replace damaged tissue.
Scientists even demonstrated that human stem cells will take root inside mice, showing their potential. The most promising outcome of this study was that stem cells do more than simply replace tissue in damaged structures. They actually create new air pathways.
This is huge news for patients with severely damaged lungs, where some structures might be resistant to repair. Knowing the mechanisms of stem cell repair, stem cell patients are probably curious about the risks and benefits as well. Are stem cell treatments really a viable option? If so, what must the patient take into account before proceeding?
Risks of Stem Cell Treatments for Lungs
Despite the promise of this type of regenerative medicine, several risks do exist for stem cell treatments. First and foremost, there is the issue of where the stem cells come from. In many cases, it is possible to harvest and reinject stem cells from the patient’s own body (called “autologous” cells).
Researchers collect the cells, isolate them, encourage their proliferation and then reinject them back into the host. Ideally, they then start to repopulate inside the patient, repairing damaged tissue and healing the organ. However, in some cases, this isn’t possible. For instance, if the patient’s own cells are too damaged, they may not have the capability to proliferate. Similarly, if a patient has a serious cancer, their stem cells carry the risk of reintroducing cancer after radiation and chemotherapy has destroyed it.
If using stem cells belonging to a patient is not an option, a patient may receive stem cells from a donor (called “allogeneic” cells). This too is a difficult prospect. Although there are basic tests performed on donor stem cells, it doesn’t guarantee that any stem cell will take. The donor must have the same blood type and doctors must conduct other types of test to ensure genetic compatibility. Even then, compatibility is no guarantee of effectiveness.
Graft-versus-host disease is one of the most serious complications. Once a physician introduces cells to a patient’s body, the donor cells (“the graft”) may attack the patient’s healthy tissues and organs (“the host”), in the same way that they would attack viruses or toxins. This can impair the tissue or organ’s function or may cause it to fail altogether. In the lungs, the two most common noninfectious problems (i.e. not related to bacterial complications) are bronchiolitis obliterans syndrome and bronchiolitis obliterans organizing pneumonia. The first is classed as a type of graft-versus-host disease and can cause issues such as diarrhea, skin rashes, liver damage, and even death.
Benefits of Stem Cell Treatments for Lungs

In case readers get the impression that the news is all bad, it’s important to convey the good news as well. Lung stem cell transplants are an exciting new approach to lung treatment. By inserting healthy stem cells in the body, patients not only receive healing potential, but a renewed capacity to fight new infections, wounds, and other traumas.
In addition to COPD, lung cancer and pulmonary fibrosis, lung stem cells may also aid in the fight against cystic fibrosis. Plus, other research hints that researchers may be able to utilize stem cells from fat tissue to help heal lungs. This would help greatly, because it would allow patients to use their own stem cells from non-damaged, non-cancerous parts of their body.
Lung Stem Cell Clinical Trials
In recent years, lung stem cell clinical trials have began to populate around the world. These trials can be searched at ClinicalTrials.gov, a website that maintains a “database of publicly and privately supported clinical studies of human participants from around the world.”
When ClinicalTrials.gov is screened for trials that involve the use of stem cells for the treatment of lung diseases, 256 results are retrieved. (*Search terms: “stem cell” OR “stem cells” | Lung Diseases”; Date: 11/02/2020). Notable companies who are sponsoring these clinical trials include:
- Athersys
- Bioheart Inc.
- Cell Therapy Catapult
- Karolinska Institutet
- And many others
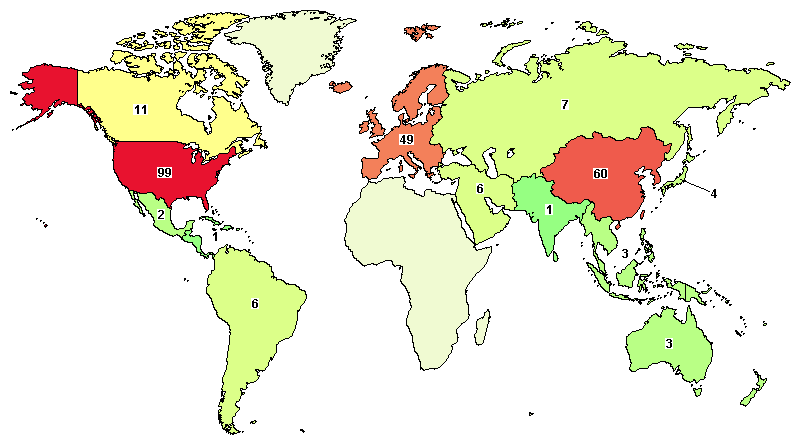
When trials using stem cells to treat lung disease are sorted by location, the U.S. (99 trials), East Asia (6 trials), and Europe (49 trials) lead the way. See a map of this clinical trial distribution below.
It may take some time for these trials to reach commercialization, but it is a momentous step to see this volume of clinical activity occurring in human patients. Patients hoping to benefit from such studies should speak with their physicians to ask about potential opportunities for their disease or condition.
Overall, the research related to lung stem cells is promising and can only get better. For those struggling with lung disease, we encourage you to keep the hope alive.
Do you have additional questions about stem cell treatments for lungs? Ask them in comments below.
Seeking advanced stem cell treatment?
RejuvStem, a premier regenerative medicine center uniquely offers proprietary Dezawa MuseCells® and Dezawa MuseExosomes®.
Unlike conventional stem cell clinics, RejuvStem combines its patented protocols, rigorously sourced, high-purity mesenchymal stem cells (MSCs) and Dezawa MuseCells® for a range of regenerative applications. Their expert medical team can evaluate whether MUSE cell therapy or premium MSC treatment is the appropriate protocol for your specific condition.
Located in Cancún, Mexico, RejuvStem Clinic serves patients from the United States, Canada, and throughout the world. Contact them today or request a free consultation.
Disclaimer: All statements made in this post are not expressed as medical claims. They are not intended to diagnose, treat, cure or prevent any disease or condition. If you have a health condition or concern, consult a physician or your health care provider. Always consult a medical doctor before using or pursuing any product, treatment, drug, therapy, or new activity.

Hi are there any clinical trial for lung stem cell treatment in INDIA.?
Are there any clinical trials for lung stem cell therapy treatment in India?
What about stem cell for advanced small cell
Looking for trials for UK?
Are there any clinical trials for lung stem cell therapy treatment in Australia?