|
|
What is the difference between an allogeneic and autologous treatment? Whether it is a stem cell treatment, a bone marrow transplant, or another type of cellular therapy, allogeneic means “from another person” while autologous means “from oneself.”
Let’s dig into this in more detail and explain why both of these approaches are commonly used within medicine.
Allogeneic vs. Autologous
There exist two types of stem cell transplant: autologous and allogeneic. Both transplants begin in the same way, with the harvest of cells from the donor’s body.
These cells undergo separation, preparation, and in some cases, a growth stage to increase their numbers. Once ready, these cells then get injected or infused into the patient’s body to heal an affected area or treat a medical condition.
With regard to allogeneic vs. autologous treatments, it it the source of the donor that creates the difference:
- In the case of allogeneic treatments, the donor is another person. While this is frequently a family member or relative, it can also be a genetically-matched donor from the general population.
- In the case of autologous treatments, the donor is oneself. Meaning, the cells are collected from the patient and then re-administered to the same person from which they were sourced.
In short, allogeneic means “from another person” while autologous means “from oneself.”
What is an Allogeneic Transplant?
An allogeneic transplant is when donor cells are collected from another person who is not the patient. Hematopoietic Stem Cell Transplantation (HSCT) is the most common example of an allogeneic transplant procedure, because it involves the use of stem cells collected from another person’s:
- Bone marrow
- Peripheral blood
- Umbilical cord blood
HSCT is a widely accepted type of stem cell transplant, because it has been performed for over 60 years. In 1965, the first successful bone marrow transplant was performed by Dr. Donnall Thomas in New York, who extracted bone marrow from a healthy twin and administered it to other twin who had leukaemia.
HSCT is usually performed for patients with cancers of the blood or bone marrow, such as leukemia and multiple myeloma patients.
Are Allogeneic Stem Cell Transplants Safe?
Unfortunately, allogeneic stem cell transplants carry the danger of graft-versus-host disease (GvHD). This is a condition in which the donor cells perceive the body as a foreign invader. Those cells set off an immune response that attacks the patient.
This is an risky occurrence, affecting between 35 and 50% of patients who undergo a hematopoietic stem cell transplant (HSCT). GVHD can cause acute symptoms, such as rash, nausea, abdominal pain, diarrhea and vomiting, and in severe cases, even death.
Allogeneic stem cell transplants may also require immunosuppressants, which are drugs that reduce the quality of the body’s immune system. Also called antirejection drugs, immunosuppressants make the patient vulnerable to infections and make any infections they get more difficult to treat.
Allogeneic stem cell transplants are also more prone to being rejected by the patient.
Autologous Stem Cell Transplants
An autologous transplant is when the donor cells are collected directly from the patient. Meaning, the cells to be administered are both collected from and given to the same person.
Graft-versus-host disease (GvHD) is avoidable with an autologous stem cell transplant, because the cells come from the patient’s own body. The donor cells will not be recognized as a foreign entity, because they come from the same person. Similarly, the patient is unlikely to reject the transplanted cells, because they are their own.
However, in some cases, contamination or other factors may make the cells unsafe and the body will attack them.
Are Autologous Stem Cell Transplants Safe?
Overall, however, autologous stem cell transplants are safer than allogeneic stem cell transplants. First, they prevent the need to find a donor, and second, they save valuable time. They also reduce the probability of side effects.
One situation in which autologous transplants aren’t a good idea is when the patient has cancer. In this case, the risk of re-transmitting it into the patient through significant. If a patient has recovered from cancer through surgery, radiation, or chemotherapy, then re-administering their cells back to them may pose an unacceptable hazard. In this case, donor cells are a better choice.
Unless the treatment strategy is a gene therapy, in which a patient’s genes are modified prior to re-administering them, it is also inappropriate to use an autologous stem cell transplant is when the patient has a genetic condition.
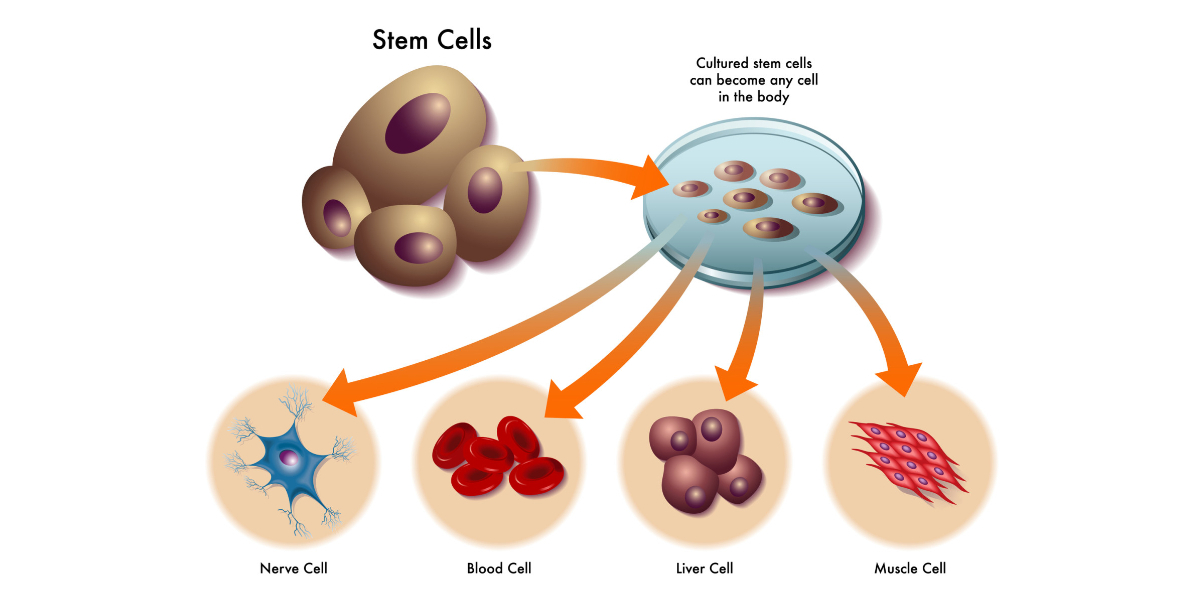
How Stem Cell Transplants Work
The infographic below depicts how stem cell transplants work, including the differences between allogeneic and autologous transplants.

Do you have other questions about allogeneic versus an autologous treatments? If so, ask them in the comments below.
Understandably, BioInformant is a publisher of stem cell industry news and cannot provide medical treatments or advice. If you have questions about your medical situation or health, we encourage you to contact RegeneVive. To date, RegeneVive’s protocols have been used to complete over 10,000+ treatments. RegeneVive’s goal is to offer cutting-edge, extensively researched stem cell therapy options.

Tell Us What You Think!